This advertorial is sponsored by VentureMed Group.
Arteriovenous (AV) access is challenging and dialysis is hard on the body and the mind. It causes physical aches, pains, and changes in the body that rob patients of energy and strength.1 When access becomes blocked, regaining blood flow can be painful, delay life-saving treatment, and lead to complications for patients over the long-term. The repetitive occurrence of access dysfunction is a persistent issue that challenges physicians and frustrates patients. Extending the time between interventions likely improves the quality of life for dialysis patients.
Percutaneous transluminal balloon angioplasty (PTA) is the standard procedure for stenoses in arteriovenous fistulas (AVFs) and grafts. This procedure will usually provide a successful immediate result. However, the lasting patency is less than optimal requiring patients to undergo frequent interventions.2 New devices, treatments, and therapies are key to making needed advancements in this disease state.
Novel non-balloon vessel prep solution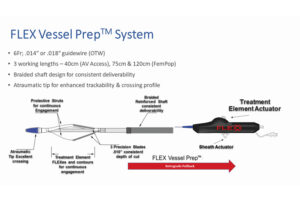
The FLEX vessel prepTM system (FLEX VP) is designed to treat AV access dysfunction. It creates micro-incisions that release the circumferential tension and improves vessel compliance and lumen gain with the intention to reduce the acute need for high-pressure PTA and associated barotrauma that may be a stimulus for restenosis.2
The FLEX VP is an endovascular medical device indicated for use prior to PTA to facilitate dilation of stenoses in the femoral and popliteal arteries and treatment of obstructive lesions of native or synthetic AV dialysis fistulae. The FLEX VP is also indicated for treatment of in-stent restenosis of balloon expandable and self-expanding stents in the peripheral vasculature. The proximal portion of each treatment element strut includes a 0.010-inch micro-surgical blade. Once the device is advanced past the lesion, the treatment element is unsheathed and expanded, and the catheter is slowly drawn back, allowing the micro-surgical blades to independently engage in the lesion and create three parallel, continuous micro-incisions, with a depth of approximately 0.010 inches along the entire length of the lesion. Once the lesion is crossed, the treatment element is re-sheathed and advanced again through the lesion, rotated approximately 30–90 degrees before the treatment element is re-deployed and the retrograde pullback described above is repeated based on operator preference. The micro-surgical blades of FLEX VP exert a consistent force of approximately 1atm on the vessel wall to deliver precise, parallel, micro-incisions addressing a wide range of morphologies.
Positive, real-world clinical data
The FLEX AV Registry study is a multicentre, prospective, observational registry (FLEX AV) enrolling haemodialysis patients scheduled to undergo PTA of their AV fistula or graft due to clinical or haemodynamic abnormalities.
One-hundred and fourteen patients across eight clinical sites were treated with the FLEX VP prior to PTA. No serious adverse events were reported. Among the 82 patients who underwent FLEX VP with plain balloon PTA, target lesion primary patency at 12 months was 44.8% with an average freedom from target lesion revascularisation of 256.6 days. Target lesion primary patency and freedom from target lesion revascularisation for AV fistula cases (n=57) were 49% and 267.3 days, respectively. In cases treating AVF cephalic arch stenosis (n=23), 12-month target lesion primary patency was 59.7% with an average freedom from target lesion revascularisation of 267.7 days.3
For reference, the FLEX VP results are favourable to the literature for treating fistulas with PTA alone. There is a large variation of target lesion primary patency results from 0% to 47.2%. The literature also shows cephalic arch lesions have documented 12-month primary patency ranging from 0% to 33.9%. In addition, it has been reported that the incidence of re-intervention in cephalic arch lesions is up to 3.5 times per year.4
Clinical utilisation with the experts

Commenting on his experience with FLEX VP, John Aruny (Musc Health, Dialysis Access Institute, Orangeburg, USA) had this to say: “I have worked with FLEX for several years as part of the growing body of evidence in clinical trials. FLEX offers a safer procedure than standalone high-pressure PTA, with no adverse events. Most recently, we published on the 12-month outcomes, which demonstrated sustained patency across most patients, and what we saw in challenging cephalic arch patients was even more impressive. Twelve-month patency for AVF lesions was 49% and cephalic arch showed 59.7% patency. Vessel Prep in AV access with long micro-incisions may also provide an attractive alternative to drug-coated balloons (DCBs) for AV access repair where cost is a key concern.”

Robert Shahverdyan (Asklepios Klinik Barmbek, Hamburg, Germany) also explored his experience with the FLEX VP: “I have used this device in my practice to treat dysfunctional AV access, and there is no other device like it due to its mechanism of treatment. It is very easy to learn and use, and takes up very little space in our lab, with two sizes available for AV access. FLEX VP creates micro-incisions along the entire length of the stenoses in significantly shorter procedure time as compared to prolonged balloon angioplasty, hence also reducing the radiation exposure time, if performed under X-ray and not ultrasound guidance only. The benefits are many, including reducing the necessity to use high or ultra-high-pressure balloons prior to using DCBs. These micro-incisions also look to potentially increase the effectiveness of drug application into the vessel wall via the use of DCBs, and seem to even reduce the pain for patients, which they experience during the traditional PTA procedures. I am impressed with the ability to clearly see the device and its instant effect on the lesion under ultrasound guidance.”
Looking forward in AV access maintenance
Chronic kidney disease (CKD) has emerged as one of the most prominent causes of death and suffering in the 21st century.5 As end-stage renal disease grows, due in part to the rise in risk factors, such as obesity and diabetes mellitus, the number of haemodialysis patients impacted by AV access dysfunction will continue to increase. The good news is that medical device innovations like FLEX VP are created to help advance patient care so that patients maintain their lifesaving haemodialysis therapy.
References
- Dialysis is not your life, The Power to redefine your life while on dialysis, Fred Hill, 2020 Reset inc.
- Aruny et al., Longitudinal micro-incision creation prior to balloon angioplasty for treatment of arteriovenous access dysfunction in a real-world patient population: 6-month cohort analysis. Hemodialysis International. 2023:1.
- Aruny J, Hull JE, Yevzlin A et al. Longitudinal micro-incision creation prior to balloon angioplasty for treatment of arteriovenous access dysfunction in a real-world patient population: 12-month cohort analysis. J Interventional Nephrol. (2023).
- Beathard GA, Jennings WC, Wasse H et al. ASDIN white paper: Management of cephalic arch stenosis endorsed by the American Society of Diagnostic and Interventional Nephrology. J Vasc Access. 24, 358-69 (2023).
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9073222/#bib1











