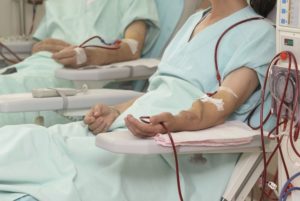
 Percutaneous endovascular arteriovenous fistula (pAVF) procedures carry a lower risk of steal syndrome and wound infection than surgical arteriovenous fistula creation (sAVF), a new study has suggested. Published in the Journal of Vascular Surgery (JVS), the review of existing data on the two procedures examines whether pAVF improves on sAVF’s patency and complication rates.
Percutaneous endovascular arteriovenous fistula (pAVF) procedures carry a lower risk of steal syndrome and wound infection than surgical arteriovenous fistula creation (sAVF), a new study has suggested. Published in the Journal of Vascular Surgery (JVS), the review of existing data on the two procedures examines whether pAVF improves on sAVF’s patency and complication rates.
The authors, led by Alkis Bontinis (AHEPA University Hospital, Thessaloniki, Greece), conducted an aggregated data meta-analysis of 18 pAVF and sAVF studies which involved retrieval of journal articles according to keywords present in their abstracts. The researchers then examined the articles for relevance before using their data. Primary endpoints were primary and secondary patency at a maximum follow-up of one year after the procedures. Researchers considered the risks of bias in their review through use of the Methodological Index for Non-Randomised Studies (MINORS) tool.
Secondary endpoints included reintervention at the end of follow-up and incidence of major complications. Steal syndrome and wound infection are two of the complications most commonly associated with AVF procedures—the study authors’ comparison of sAVF and pAVF finds that there was “an almost sixfold increased risk for steal syndrome occurrence” when a fistula is created through sAVF instead of pAVF.
The researchers suggest that it is pAVF’s standardisation of the size of the fistula that accounts for this difference, which stands in contrast to sAVF’s reliance on “the surgeon’s subjective perception” of appropriate size. sAVF also demonstrates low primary patency rates and a higher rate of reintervention. The primary endpoints, however, do not show statistically significant differences between pAVF and sAVF.
The medium quality of the studies used in the authors’ meta-analysis is described as a limitation. Other limitations include the fact that the studies examined are retrospective and that only five out of the total 18 analysed directly compared the two procedures. The authors are keen to note also that “the high heterogeneity presented in our results reflect variation in surgical strategies, anatomic locations, learning curve requirements and individual surgeons’ abilities.”












