 Transplant experts at Hackensack University Medical Centre have been the first in the USA to use new kidney preservation technology that can expand the window of time in which a kidney is viable—reducing the time it takes to receive a kidney transplant.
Transplant experts at Hackensack University Medical Centre have been the first in the USA to use new kidney preservation technology that can expand the window of time in which a kidney is viable—reducing the time it takes to receive a kidney transplant.
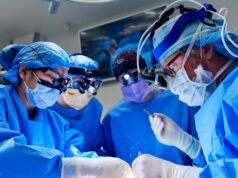
Now the team is evaluating this approach to see if it extends the lives of donated organs, and whether it can thus expand the number of donor kidneys that are viable for transplantation, helping to address the organ shortage in the USA. The technology, known as the Kidney Assist device (XVIVO), works by keeping a donated kidney warm, functioning, and supplied with nutrients outside of the body prior to transplant. Doctors use the experimental device to supply blood and oxygen to a human kidney at normal body temperature.
For decades, kidneys donated for transplantation by a deceased donor have been transported on ice in coolers until they reach the transplant recipient. While this puts the kidney into a “hibernation” mode, suspending its ability to function, it does not supply the oxygen and nutrients the organ needs and can result in organ damage—limiting the lifespan of the kidney outside the body. “Organs want to be treated the way our bodies treat them—warm and protected, with blood and oxygen,” explained Michael Goldstein, director of the Division of Organ Transplantation at Hackensack University Medical Center (Hackensack, USA), who performed the Kidney Assist study.
The hospital is the only one in New Jersey to routinely perform kidney transplants with machine perfusion technology. Since 2020, doctors have used an ex vivo machine preservation technology that increases a kidney’s lifespan under hypothermic (cold) conditions, improving patient outcomes. The new Kidney Assist technology is a step up from that approach, perfusing the donor kidney with blood and oxygen under normal body temperature (warm) conditions. The kidney that Goldstein and his team connected to Kidney Assist produced 200ml of urine, indicating that it was functional and healthy and supporting its potential use for transplantation. Kidney Assist may convert organs that may have previously been rejected into usable kidneys for transplantation.
Goldstein and his colleagues will continue to assess the normothermic technology to see if it improves kidney parameters. They also plan to draft guidelines detailing how to interpret the data to determine if a kidney is viable for transplantation. “Kidney Assist may enable us to salvage more organs, keep them out of the body longer, deliver them more safely to the people who need them, and increase the number of organs available for transplantation,” he concluded. “Our goal is to get this technology approved for use in the United States so we can save more organs and save more lives.”