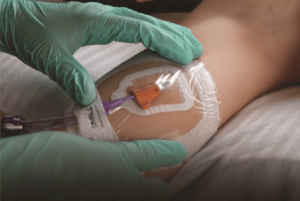
 The largest study ever conducted of patients with peripherally inserted central catheters (PICCs) utilising a subcutaneous anchoring securement system (SASS) has found that using subcutaneous anchors to secure catheters is more effective than using adhesive securement devices (ASD).
The largest study ever conducted of patients with peripherally inserted central catheters (PICCs) utilising a subcutaneous anchoring securement system (SASS) has found that using subcutaneous anchors to secure catheters is more effective than using adhesive securement devices (ASD).
The retrospective study was conducted at The Clatterbridge Cancer Centre (Liverpool, UK) and published in the Journal of Vascular Access. It compared the outcomes of using different securement systems in more than 9,200 oncology patients, covering more than a million catheter days in the period 2009–2020.
A significant outcome of the study found that adhesives devices put patients at 36 times greater risk of partial or complete dislodgement of their PICC compared to a subcutaneous anchor.
The results were clear and impressive, say co-authors Carol McCormick (Clatterbridge Cancer Centre), and Michelle Hawes, president of the Association for Vascular Access Foundation. Twelve percent of patients with catheters held in place with adhesives required unplanned catheter replacements, compared to only 0.4% of patients with the subcutaneous anchor.
Prior to the implementation of SASS, only 77% of the oncology patients made it to the end of need for their PICC without a replacement required. By 2020, 99% of the patients with a subcutaneous anchor holding their PICC finished their course of need with one catheter. “Based on the evidence, the best instrument for securing a catheter throughout a patient’s therapeutic need is the subcutaneous anchoring securement device,” says Hawes.
The study suggests that switching to the subcutaneous anchor can both improve patient outcomes and reduce overall healthcare costs. A press release notes that thousands of central venous access devices (CVADs), including central venous catheters (CVCs) and PICCs, are inserted into patients every month.
Historically, it goes on to say, the standard medical practice has been to secure most central venous catheters with sutures and most PICCs with an ASD; while a SASS has been available for nearly two decades, many health professionals are not familiar with its use.
When McCormick first introduced the subcutaneous anchor device used in the study to Clatterbridge, “the majority of nurses were fearful of the device,” she recalls. Since then, its use has grown. It is now used in more than 100 National Health Service (NHS) facilities across England. However, until this new retrospective study, there has been little conclusive evidence on which securement methods actually prevent partial or complete dislodgement.
Both McCormick and Hawes hope that the evidence from the new study will accelerate the adoption of the device, currently the only subcutaneous anchor securement system, reducing unplanned catheter removals, complications, and improving patient outcomes. They also expect that the increased use of the devices will bring significant cost savings, despite higher upfront costs, because only one device is required until the catheter is removed unlike all other engineered securement devices, including ASDs. Additionally, a secure catheter will lower hospital readmissions and reduce the need for multiple lines to complete therapy. Indeed, a review by an advisory committee of the UK’s National Institute for Health and Care Excellence (NICE) estimates annual savings at more than £4.2 million.
The new retrospective study adds to a “growing body of research” showing benefits of subcutaneous anchor devices, including a 2020 study that showed reduced risk of bloodstream infections and a 2022 study that evaluated safety and efficacy outcomes for CVAD securement options. Hawes will present the new data at the upcoming Association for Vascular Access 2023 Annual Scientific Meeting, (October 14–17 2023, Portland, USA). Her presentation, “Keep it Simple Specialist: One Securement Device, One PICC, Until the End of Need,” will take place on 15 October at 1 pm Pacific Daylight Time (PDT), the release concludes.












