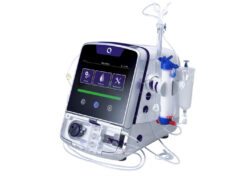
It’s possible to expand the action radius of a passion for kitesurfing, despite being on long-term dialysis. Pascal Kopperschmidt (Hamburg, Germany) gave attendees at the 5th Hamburg Dialysis Access symposium (8–9 September 2023; Hamburg, Germany) a glimpse of the risks and promises of self-care from a patient’s perspective.
It’s possible to expand the action radius of a passion for kitesurfing, despite being on long-term dialysis. Pascal Kopperschmidt (Hamburg, Germany) gave attendees at the 5th Hamburg Dialysis Access symposium (8–9 September 2023; Hamburg, Germany) a glimpse of the risks and promises of self-care from a patient’s perspective.
In a talk titled “true crimes: an unforgettable night”, Kopperschmidt, a physicist in the medical device industry, and a patient with 35 years of dialysis experience—of which the last 25 have been on home haemodialysis—delivered a flavour of his “nightmare scenarios” framed by stories and anecdotes of a life lived to the full while needing to be on dialysis.
Kopperschmidt has been a long advocate of self-care and has published several articles on the topic. “Self-care, whether in the home environment or a limited-care dialysis centre, empowers patients by allowing them more treatment autonomy. The choice of home rather than in-centre haemodialysis may be driven by, among other reasons, a demand for technically intensive care in a less formal environment,” he writes with co-authors. His mantra has often rested on the idea that “increasing individualisation of treatment at home often accompanies patients growing in self-confidence and experience of managing their own care.”
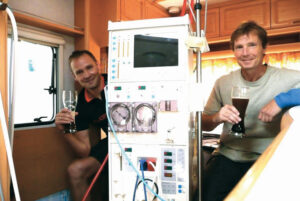
able to dialyse in different, sometimes unconventional locations
Returning to the question of nightmares, he treaded lightly on the lows. “Putting a haemodialysis machine into a camper van might well represent a nightmare to some,” he said, explaining that he saw dialysing at different locations as a way to extend the action radius of his passion for kitesurfing—this made the dialysis machine in the camper van, a reason to celebrate. “When you have something to celebrate, you must celebrate,” he urged.
Kopperschmidt displayed images of a dialysis machine in a tent in the Australian outback, revealing that this was shared with a friend for a couple of weeks in a national park (a nightmare for their wives, but not for us, he said). He then pictured a “temporary dialysis unit in a barn in the north island of New Zealand equipped with two dialysis units (a nightmare for the cows and roosters running around the barn and wondering what was going on there, which was two guys having dialysis, he qualified), as well as the tiniest dialysis centre in the world: a Volkswagen bus, equipped with a dialysis machine, a narrow bed and space left for kitesurfing paraphernalia.
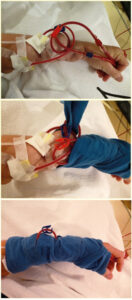
There are, of course, also clear risks associated with dialysing in both conventional and unconventional locations, and Kopperschmidt outlined these as well. “Self-punctures are a nightmare for many, many patients, but when you use the right technique, e.g. the buttonhole technique with the right needles, and yes, the right mindset, it’s absolutely not a nightmare to put that needle into that tiny hole, every other day. I’m on eight-hour nocturnal dialysis every other day, otherwise I probably wouldn’t be here,” he said, making the point that nocturnal haemodialysis, both in-centre and at home, allows for the delivery of more intensive haemodialysis, greater freedoms and better quality of life.
But these eight hours can be an ordeal, he cautioned, especially when the venous needle gets repositioned, or removed overnight unnoticed. “The venous dislodgement of the needle [is a case in point], but I have found a technical solution to that by using a bandage. Here the blood tube attached to the needle is guided into a loop. The bandage wrapped around the fistula site penetrates the inner eye of the loop to fix the loop, not the line. An accidental strong pull at the line forces the loop to reduce its diameter, leading to a kink that is noticed by the dialysis device pressure unit. The needle itself, however, remains on the spot” Kopperschmidt said. “It’s crucial to think about what happens overnight when the needle is disconnected. This bandage technique is safe and easy to apply and prevents patients from being injured by massive blood losses.”
Kopperschmidt also called for awareness amongst patients on home haemodialysis of albumin loss or protein loss from long dialysis treatments. “When you understand that the protein sieving coefficients of dialyser membranes significantly decline within the first 20 minutes of a treatment, the difference in protein loss comparing long-term dialysis sessions with standard becomes negligible,” he said.
 Turning to his zeal for kitesurfing, he displayed a gravity-defying image of himself kitesurfing to suggest this might be scary—to be at the mercy of strong winds and high waves, riding the tide on a tiny boat. “Some might see this as a time for the last prayer, but gaining the third dimension is not a nightmare,” he clarified, despite then going on to describe a situation when inevitable malfunctioning of kit can cause blood loss to soar, which definitely qualifies as much worse than a bad dream.
Turning to his zeal for kitesurfing, he displayed a gravity-defying image of himself kitesurfing to suggest this might be scary—to be at the mercy of strong winds and high waves, riding the tide on a tiny boat. “Some might see this as a time for the last prayer, but gaining the third dimension is not a nightmare,” he clarified, despite then going on to describe a situation when inevitable malfunctioning of kit can cause blood loss to soar, which definitely qualifies as much worse than a bad dream.
A Duni connector from the dialysis machine with an undetectable tiny overnight leak, for isntance, once caused severe blood loss. “After roughly seven hours, I woke up and couldn’t really move or say much. When trying to calculate the amount of blood lying on the floor, I guess it was about two litres,” Kopperschmidt added. “At the end of the day, I was transferred to an emergency unit for substitutional volumes and it took me six months to get to previous iron and haemoglobin levels.
“I recovered, as you can see; this was many, many years ago. You can imagine what that blood on the floor looked like; it was a night to remember.”
Course director of the Hamburg Dialysis Access symposium Robert Shahverdyan (Hamburg, Germany) told Renal Interventions: “Pascal has been a home haemodialysis patient for many years, with a truly impressive backstory. He is a good friend and has been one of the speakers at our symposium, every year since I started it back in 2008. When I was planning the case session called “My worst nightmare—cowboy up!” last year, it was only logical to invite Pascal to give us an exciting story from his long home haemodialysis experience, which he did incredibly.”