An observational study published in the Journal of the American Society of Nephrology (JASN) has identified a “promising” histological marker for determining kidney transplant failure. A collaboration between Kyoto University and Akita University in Japan—led by Motoko Yanagita, a professor in the Department of Nephrology and the Institute for the Advanced Study of Human Biology (ASHBi) at Kyoto University, Kyoto, Japan—has found a common but previously unappreciated observation of kidney grafts, which is that tertiary lymphoid tissues may prove a valuable prognosis marker in transplant outcomes.
“Graft survival in the short-term has greatly improved in the last three decades, but long-term survival has only improved marginally,” said Yanagita.
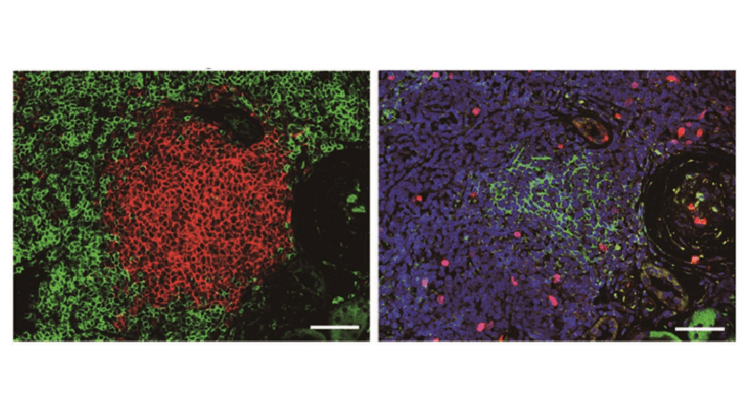
One of the key indicators of a failing transplant is inflammation. Commonly accompanying the inflammation are tertiary lymphoid tissues, which the study describes as “inducible ectopic lymphoid tissues that arise in chronic inflammatory conditions such as ageing, cancer, autoimmune disease and transplanted organs”.
Tertiary lymphoid tissues are essentially a natural development of ageing and the associated health burdens that come with it. However, while the medical community is well aware of the appearance of tertiary lymphoid tissues in kidney transplants, there is little understanding about their role in graft survival.
One reason the significance of tertiary lymphoid tissues had been ignored was that doctors and scientists had not appreciated the different stages of the tissues, a statement from Kyoto University notes. Last year, Yanagita’s team reported two stages distinguished by the absence (stage I) and presence (stage II) of follicular dendritic cells—a natural type of fibroblasts found in the human body.
The new study examined 214 kidney transplant patients who showed no rejection. Each patient underwent kidney biopsies immediately, and one, six and 12 months, after the transplantation to ensure no rejection. Tertiary lymphoid tissues were hardly seen immediately after the transplantation but were already present in about half after one month.
Stage II tertiary lymphoid tissues, however, were only found in less than 10% of biopsies after six months and in almost 20% after one year. Those patients whose biopsies showed stage II tertiary lymphoid tissues also had a much higher likelihood of renal failure within five years of the transplantation too. “The patients with stage II tertiary lymphoid tissues showed a higher risk of future decline in graft function,” Yanagita added.
Moreover, she claimed, the presence of stage II tertiary lymphoid tissues did not necessarily associate with the inflammatory score of Banff classification, which is a standard scoring system used by clinicians to grade biopsies from solid organ transplants. Instead, the stage II tertiary lymphoid tissues may provide another useful diagnostic marker of graft survival in kidney transplantation.
“Stage II tertiary lymphoid tissues were observed in graft tissues that had mild interstitial inflammation,” Yanagita concluded. “These findings suggest that tertiary lymphoid tissues are qualitatively different from simple interstitial inflammation and might be regarded as novel histological markers of graft outcomes.”